Radiation therapy is an allied health profession which employs radiation in the treatment of disease, especially cancer. The Bachelor of Science in Radiation Therapy is a four-year, “2+2” program. Students first complete two years of liberal and pre-professional science education courses at the University of St. Francis, followed by two years of professional coursework and clinical education at an affiliated hospital or cancer center.
The curriculum is designed to provide for balanced didactic and clinical components in order to produce students with a well-rounded education in radiation therapy. Successful completion of the professional education component of the program, makes the graduate eligible to take the national certification examination of the American Registry of Radiologic Technologists (AART).
The job outlook for radiation therapists continues to be promising. According to the U.S. Department of Labor Statistics, employment in the field is projected to rise 2% from 2024-2034. As the population of our country ages, the need for radiation therapists will likely increase. The median annual wage for radiation therapists was $101,990 in 2024.
Students are accepted into the professional sequence of courses every spring and begin coursework in the fall semester. Applications into the professional component are due by December 15 yearly.
Admitted Student Statistics:
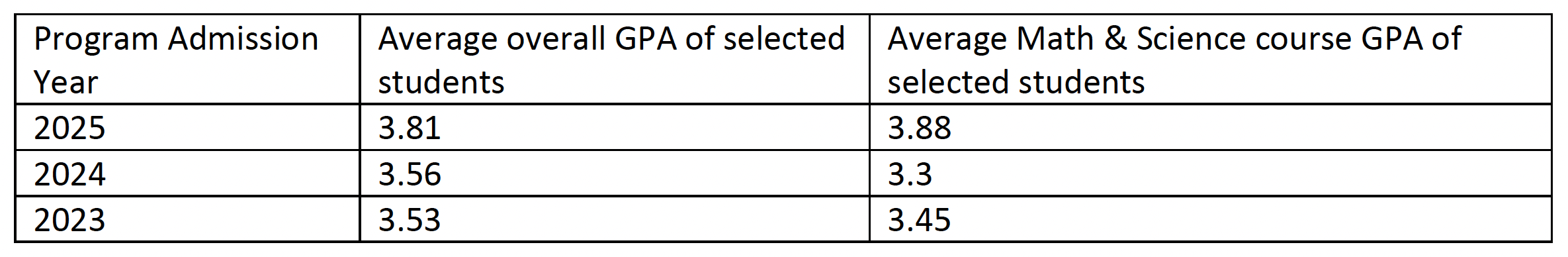
Mission:
The mission of the Radiation Therapy Program is to provide academic, clinical and professional education of exceptional value to students, and to graduate radiation therapy students with the technical abilities, as well as the cognitive, critical and analytical thinking skills desired by employers such that graduates are prepared to serve at entry level and advance to leadership positions.
Toward fulfillment of our program mission, there are four main goals with focus toward student learning and four main goals focused toward program effectiveness….
Student Learning Goals and Expected Outcomes:
1. Facilitate clinical competence such that students may:
a. Demonstrate technical knowledge and skills commiserate with level of education
b. Demonstrate cognitive abilities appropriate to level of education
c. Integrate and apply theories and principles to final semester physics assignments
2. Foster and develop critical, analytical and problem solving skills such that students may:
a. Show progressive, relative proficiency in describing rationale for therapy planning during simulation by procedure journaling
b. Show progressive, relative proficiency in describing rationale for treatment delivery
c. Show progressive, relative proficiency in describing rationale for therapy planning during simulation by oral examination
3. Foster and develop oral and written communication skills such that students and/or graduates may:
a. Orally present concepts with progressive, relative proficiency in content, organization and delivery
b. Successfully conduct written research on topics related to radiation therapy
c. Demonstrate effective communication skills with patients, peers, and team during internship
d. Demonstrate effective communication skills with patients, peers, and team as program graduate
4. Instill ideals supportive of professional growth and development such that students and/or graduates may:
a. Successfully prepare and display campaign for career promotion and patient advocacy
b. Demonstrate professional characteristics in the workplace as program graduate
Program Effectiveness Goals and Expected Outcomes:
5. Maintain an optimal teaching and learning environment such that students and/or graduates may:
a. Express satisfaction with the overall quality of instruction in online and traditional delivery formats
b. Express satisfaction with overall quality of clinical education
c. Express satisfaction with received advice, mentoring and counseling provided by clinical supervisors
d. Communicate satisfaction with overall quality of education by being willing to recommend by program end
6. Employ admissions processes with the greatest potential for academic success and program completion such that students may:
a. Successfully complete all program requirements within 150% of program length
b. Successfully complete all didactic courses above minimum admissions academic standard
7. Facilitate professional practice preparedness such that students, graduates and/or employers may:
a. Demonstrate technical and clinical skills with minimal supervision in final semester
b. Express overall satisfaction with program as perceived post-graduation
c. Describe the benefits of professional organization membership, licensure, certification and scholarly activity
d. Express overall satisfaction with level of preparedness shown by employed graduates
8. Demonstrate acceptable national registry examination pass rates and favorable job placement by students and/or graduates who are able to:
a. Apply all radiation therapy principles for successful performance on comprehensive examinations
b. Successfully pass the national registry examination on the first attempt within six months of program completion
c. Perform above national and state means on the national registry examination
d. Obtain employment within six months of program completion
A detailed description of goals, outcomes, measurement tools, and measurement frequencies is found in the program’s 3-year Outcomes Assessment Plan.
The clinical education portion of the program is designed to assure that graduates are prepared to successfully complete the ARRT exam in radiation therapy, meet licensure requirements, and assume the duties and responsibilities of an entry level therapist.
General clinical course requirements are reviewed during program orientation. Clinical course requirements and expectations specific to each semester are reviewed at the start of the semester. Students will be assigned to 2-3 affiliated sites during the program to maximize the potential for exposure to a variety of case types and varying departmental dynamics. The program clinical coordinator will work closely with each student to plan clinical assignments intended to foster a diversified clinical experience.
Students will spend time in the following areas of the radiation oncology department at each assigned site:
Students will be expected to spend some time away from patient care areas to complete all clinical course requirements such as case studies, cancer conference and support group journaling.
Supervision
A clinical supervisor is designated for each affiliated clinical site. Further, each student is assigned to at least one clinical instructor during a rotation through each department area. Students are under the direct supervision of their clinical instructor and are evaluated periodically by instructor(s) and supervisor. The student shall report to his/her clinical instructor at the beginning of each clinical day. It is the students’ responsibility to inform the clinical supervisor and instructor of any scheduled class or activity, which will require release from the clinical area. Under no circumstance will a student be substituted for paid staff nor take on the responsibilities of staff in the clinical area.
Evaluation
Components of clinical course evaluation include: completion of semester specific clinical objectives, performance evaluations, clinical competency examinations, simulation journals, case studies and laboratory assignments. More detailed information may be found in course syllabi for RADT 305-406 Radiotherapy Clinical Experience I- IV. Translation of clinical clock hours to semester hours follows the formula: 100 clock hours~1 semester hour.
Affiliated clinical sites include:
Advocate
Javon Bea Rockford Memorial Cancer Center: Rockford, Illinois
Joliet Oncology Hematology Associates, Ltd.: Joliet, Illinois
Morris Cancer Center: Morris, Illinois
North Shore University Health System
Riverside Cancer Institute: Bourbonnais, Illinois
SSM Health St. Mary’s Hospital: Janesville, Wisconsin
University of Chicago Radiation Oncology Center/University of Chicago: Chicago, Illinois
University of Chicago Radiation Oncology Center/Orland Park: Orland Park, Illinois
University of Chicago Medicine Comprehensive Cancer Center-Silver Cross Hospital: New Lenox, Illinois
The University of St. Francis is accredited by the Higher Learning Commission (hlcommission.org), a regional accreditation agency recognized by the U.S. Department of Education. The University of St. Francis is authorized to operate as a post-secondary educational institution by
The Illinois Board of Higher Education (ibhe.org).
The Radiation Therapy program is accredited by the Joint Review Committee on Education in Radiologic Technology (JRCERT). This certifies that the program meets or exceeds national standards for quality educational programs.
The Radiation Therapy program was reviewed by the JRCERT February 2020 and received maximum accreditation award of eight years. The next scheduled review is tentatively scheduled for the first quarter of 2028. Further information or inquiries about accreditation of the radiation therapy program may be obtained by contacting the JRCERT at 20 N. Wacker Dr., Suite 2850, Chicago, IL 60606-3182, by phone 312-704-5300, jrcert.org, or by e-mail: mail@jrcert.org. General program accreditation information and the current accreditation award letter can be found here.
–Lisa Ringstmeyer ’16
Radiation therapists work with radiation oncologists and physicians in planning and delivering the course of treatment for each patient. Radiation therapists are responsible for implementing the daily administration of prescribed doses of radiation for treatment, as well as performing calculations for the correct patient dosages. Because radiation therapy procedures are planned in advance, most radiation therapists work a day-shift schedule, and there is rarely the need to work night shifts, on weekends or on holidays. Employment opportunities for radiation therapists are in hospitals, private practice offices, outpatient centers, and comprehensive cancer centers.
The mission of the Radiation Therapy program at the University of St. Francis is to provide academic, clinical and professional education of exceptional value to students, and to graduate radiation therapy majors with desired, required, entry-level employment skills. As part of the curriculum, students will complete four radiotherapy clinical experiences over the course of four semesters. During this period, students will gain hands-on experience in the field at an affiliated clinical site, working with patients and professionals. Additionally, dedicated faculty with years of professional experience guide students throughout the program, helping students become top qualified radiation therapists.